
My eyelids fluttered. Slowly, the room came into focus. As a male nurse called out my name, I remembered. Earlier that day, I was lying flat on a cart on my way to the operating room. Along the way, I drifted off to sleep. Before I regained consciousness, my surgeon and his physician assistant had operated on my shoulder. As I became aware of my surroundings, I entered the Subacromial Decompression Post-Op recovery phase.
Prior to the surgery, I had been given two options for anesthesia- a nerve block or a general. While an effective nerve block would provide more pain relief during the first 24 hours, I opted for the general anesthesia. I had never experienced any issues with general anesthesia, but I was leery of some of the possible side effects of a nerve block. Most important was the fact that I was optimistic that my post-op pain levels would be manageable.
My post operative pain threshold is affected by my prior surgical experiences. I assumed that this shoulder surgery would be far less painful than my previous abdominal surgeries and two hip surgeries. Thus, my expectations of extreme pain were decreased. Moreover, the anesthesiologist assured me that if my post-op pain was excessive, he could administer the block before I left the surgical center.
Fortunately, during the first 24 hours, my pain was controlled by a prescription of hydrocodone/acetaminophen and the use of an ice machine. Less than 36 hours after the surgery, I experienced flushing in my face and neck. This annoying situation vanished after eliminating the narcotic drug. The portable ice machine became a constant companion and aided my recovery process. I considered myself lucky that I could get by with an occasional Extra Strength Tylenol capsule.
Less than 24 hours after the procedure, I returned to the surgeon’s office for my first post-op and physical therapy visits. The thick surgical dressing was removed. I was also instructed on post wound care and what I should and should not do.
Afterwards, the physical therapist took range of motion measurements and showed me how to do a handful of simple exercises. The exercises focused on my hands, wrists, elbows, neck, and shoulder.
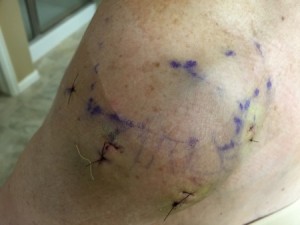
Four days after the surgery, my husband changed the waterproof bandage. I was pleased to see that there was minimal swelling and bruising. The surgeon’s marks were more prominent than the scars or the bruising.
During the next two weeks, I was given a few more exercises.

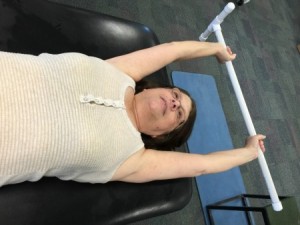
After just a few days, I could perform the overhead flexion with minimal discomfort.
I diligently followed the doctor and physical therapist’s protocols. After completing the Subacromial Decompression Post-Op recovery phase, I am sharing 10 tips for a successful recovery.
10 Tips for a Successful Subacromial Decompression Post-Op Recovery
- Acknowledge Pain/Symptoms and Treat Accordingly
Pain levels need to remain under control. Prescribed narcotics, over-the-counter drugs, and ice should be used according to an individual’s pain tolerance and doctor’s instructions. Unless instructed otherwise, take all medication with food to avoid GI related issues. A stool softener may be needed to avoid constipation that is caused by some narcotics. Unusual symptoms and/or extreme pain needs to be reported to the doctor’s office. It is better to be proactive than to suffer unnecessarily.
- Rest
The healing process will be stymied by insufficient sleep. Sleeping in a recliner may end up being the best option. Lying on the opposite side with a pillow cradled between your arms is a secondary option. Avoid sleeping in any position that causes significant pain. Finding a comfortable position in this early phase may be challenging. Napping during the day may help offset sleepless nights.
- Remain Hydrated and Eat a Balanced Diet
It is wise to flush out all of the drugs administered during surgery. Don’t forget to drink water throughout the day. Coconut water is an expensive secondary option. A decreased appetite should not be an invitation to eat junk food. Fresh fruits and vegetables as well as a fiber rich foods will help to offset the likelihood of constipation. Don’t forget to include sufficient amounts of protein into your diet.
- Follow Wound Care Directions
Until the stitches are removed, the small incisions need to be kept dry and clean. Try to avoid sweating excessively. When showering, protect the waterproof bandages with Saran Wrap or a plastic bag. Change the dressings according to the doctor’s instructions.
- Wear Comfortable Clothing
Roomy button down shirts provide the easiest access. Strapless bras may be a challenging for a well endowed woman, but will not irritate the healing wounds. Take a pass on any garment that requires your arm to go above your head or behind your back. Select shorts, pants, and/or skirts that require minimal work to get on and off.
- Initiate and Maintain Physical Therapy Protocol
Oftentimes PT will increase one’s pain level. Taking pain medication prior to a session and icing afterward will lessen this likelihood. Establishing and following a daily routine will aid in the recovery process. If the pain level exceeds what is anticipated, do not hesitate to contact the physical therapist or the doctor’s office.
- Include Daily Activity
Unless instructed by one’s doctor to remain sedentary, it is essential that you take time to move around. Weather permitting, it is advisable to go outside for a leisurely walk or remain inside to ride a stationary bicycle. A five minute walk around the house or up and down the stairs can make a huge difference. However, one should avoid sweating excessively or congested areas where one could easily be knocked into by another person.
- Wean Off Sling
Orthopedic surgeons and/or physical therapist will provide the time frame for becoming less dependent on a sling. The weaning process is dependent on the complexity of the surgery and individual recovery process. Finding one’s comfort zone is the key. After prolonged time in a sling, the arm starts to lose its flexibility and strength. Adhering to the PT protocol will help minimize any future issues.
- Avoid Painful Movements
Shoulder surgery causes different degrees of pain. Post-op instructions usually include a list of movements that should be avoided. If you are uncertain, don’t be afraid to ask. One should also be cognizant of the movements that exacerbate the discomfort.
- Maintain Positive Outlook
Emotions and mental outlook affects one’s recovery. It is easy to feel out of sorts when one’s life is temporarily limited due to the aftereffects of surgery. In order to instill a positive perspective find sufficient time to listen to music, watch comedies, read inspirational literature, and/or meditate.
Rehabbing Process Moves to Next Step
Eleven days after my surgery, the stitches were removed.A few days before my follow up visit, I had already discarded the sling. It would be a few more days before my incisions could be fully immersed in water or coated with lotion. My support stockings were no longer necessary.
I was instructed to be careful as I entered the next phase of my recovery. My arm motions were to be limited to the area immediately in front of my waist. Carrying more than a few pounds was not advised. While I never considered a container of milk to be heavy, it was now on my prohibited list. I was given the green light to drive. For the time being, I would have to focus on leading with my left arm. Shifting the car’s transmission with my left hand was awkward, but less painful than using my right arm. I started to count down the days before I could sleep through the night without waking up in pain.
Even though I have graduated to the next stage, I am following a few of the above mention tips as I return to my normal day-to-day activities.
***Sometimes life throws curve balls. Even though I meticulously followed all of the post op and physical therapy protocols, I experienced two challenging setbacks. If you find yourself in a similar predicament, consider reading Overcoming a Physical Therapy Setback
I send my best wishes to anyone who is contemplating or has recently undergone subacromial decompression shoulder surgery. Also, if you know anyone who is fed up with knee pain and considering medial meniscus surgery, please forward the following link– Should a Middle Aged Person Have Medial Meniscus Surgery
Please feel free to share any tips you have in the comment area below.
Related Blogs
10 Tips For Foot Surgery Post-Op Recovery
Can Your Diet Influence COVID-19 Immunity?
Why We Get Sick: Showcases Linkage Between Insulin Resistance and Chronic Illness
Tips for Multiple Doctors’ Opinions
6 Tips for Eliminating Back and Sciatica Pain
Should a Middle-Aged Person Have Medial Meniscus Surgery?
Overcoming a Physical Therapy Setback
Confronting an Irrational Fear
Meaningful Anniversary (hip replacement)
5 Ways to Improve Exercise Motivation
Letting Go of the Past (Momster blog on Family Circle Website)
Living Without Regrets (Momster blog on Family Circle Website)
Bio
Sandra Bornstein is the author of MAY THIS BE THE BEST YEAR OF YOUR LIFE. It is available on Amazon.
Sandra’s memoir highlights her living and teaching adventure in Bangalore, India. She is a licensed Colorado teacher who has taught K-12 students in the United States and abroad as well as college level courses. Sandra is married and has four adult sons.
The memoir was a finalist in the Travel category for the 2013 Next Generation Indie Book Awards, the 2013 International Book Awards, the 2013 National Indie Book Excellence Awards, 2013 USA Best Book Awards, and a Honorable Mention award in the Multicultural Non-Fiction category for the 2013 Global ebook Awards.
Very useful. I am 5 weeks post op, still can’t lift my arm fully, very painful especially in the bicep but taking medication still plus shoulder still very tight. Physio going well. Can run on treadmill and bike in gym. How long did it take to be pain free. Articles say 4 months.
Janet,
Thanks. I’m glad that my blog was helpful. I know that it is sometimes hard to find certain info.
Yes, textbook cases usually have a 4 month recovery time. I’ve had numerous orthopedic surgeries and know from experience that there are many factors that may speed up or slow down the rehab process.
In my case, the progress had peaks and valleys, but everything looked okay as I was approaching the 4 month mark. Without any warning, I slowly lost my range of motion and started to feel intense pain. Ouch!
I returned to the doctor. I was diagnosed with a frozen shoulder. I reluctantly agreed to a shot. I felt that it wasn’t worth dealing with a new round of pain and limited range of motion for an extended period of time. At first, the pain got worse.I wasn’t a happy camper.
I’m 3 weeks post injection and I’m now beginning to regain my range of motion and have minimal discomfort. I’m hoping that I will soon be able to put this shoulder stuff behind me.
Let me know if you have any other questions. Good luck! I hope that you’re able to return to your normal life soon.
My husband is getting shoulder surgery next week, and I want to be prepared with everything I need to take care of him. I love the idea of an ice machine, so that it stays cold for longer, and it’s really cool how it circulates around the pad. He is going to need ice for a while, and I think that is a great way to go!
Jackie,
The ice machine is vey useful. It is much better than traditional ice packs. I hope that your husband’s recovery is quick and uneventful. If anything doesn’t seem quite right, he should communicate his concerns with his doctor.
Sandra please could you contact me via email. Just needing to ask some questions about my surgery that has been proposed. It’s arthroscopic capsule release, MUA and subacromial decompression all in one go!
Paula, I hope that my email response helped. Good Luck!
I had a decompression and capsule release last year , partly successful.
I was very bruised after and not too much pain , but the nights were worse.
I had 6 weeks of physio and regained all my movement in that time,but still had a niggle when lifting my arm vertically to 12 o’clock.
It’s still jiggling me ,10 months post op no just been back to the consultant after an ultrasound show if there is fluid and still some impingement.
So I have to have it done again.
He said that when they do both a capsule release and decompression, they tend not to decompress too much.
Most people are fine, but I was unlucky.
I’m not too concerned as my movement is full range ,so o know I’ll get it back again, but this time hopefully with no glitches.
Hope that helps
Thanks for sharing. I know from personal experience that setbacks can occur. I like your positive attitude! It will help you get through the next procedure.
Good luck and let us know how things go. I’m currently rehabbing from an unrelated orthopedic surgery and secondary issue so I know all about how luck affects us all.
Thanks for the tips. My subacromial decompression, distal clavicle resection and possible rotator cuff repair (the part which I hope to avoid) are scheduled for 8 days from now. I had depcompression done (same shoulder) 15 years ago and while I remember and know much of what to prep & expect (doesn’t hurt that I’m an RN), my experience certainly isn’t fresh in my memories. Hope you’re doing well now. My last shoulder surgery was successful and my PT uneventful. That and your memory refresher gives me some confidence going into this. 🙂
Deanna,
Good luck!
I understand the uneasy feeling that one gets prior to surgery. Prior surgical experience does help, but it can’t totally eliminate the natural hesitations. I’m happy to report that my shoulder surgery was a total success. I’m so happy that I can swim and do everything that I need to do with my arm.
Unfortunately, I’m currently dealing with orthopedic foot issues that have caused a hiatus from activity. Once again, I’m looking forward to being pain free.
If you remember, add a comment after your surgery to encourage others to go forward.
Thanks for the tips Sandra!
I am 12 days out from subacromial decompression surgery. Surgeon said it went well and my shoulder is in perfect condition. He said there was a large bone spur that he shaved down.
My ROM is pretty good, I could lift my arm above my head a week after the surgery.
I’m currently doing theraband exercises and just stretching it.
I am a firefighter so I am hoping to get back to full strength ASAP.
Just wondering how long it took you to feel like you were back to full strength?
Hi Ryan,
I’m glad that your recovery is going well. Initially, my recovery was amazing and my doctor and physical therapist were thrilled.
At about 6-7 weeks, I drove 4.5 hours for a business conference and then did the return trip a few days later. Taking notes and sitting for 3 consecutive days increased my discomfort significantly. This situation wrecked havoc with my daily icing routine and daily exercises. My shoulder became more painful. It went back on track after I resumed my icing routine and PT.
A month or two after the conference, my range of motion started to diminish. I couldn’t pinpoint a cause. Once again, I had trouble putting on a jacket, doing simple movements, and increased pain in the nighttime. It was similar to some of the pre-op symptoms. When my physical therapist hit a road block, I returned to the doctor.
Surprisingly, I was diagnosed with frozen shoulder.This is an uncommon post surgical issue for this type of surgery. I was given the option of waiting a long time for it to heal on its own (1-2 years) or consent to an ultrasound guided cortisone shot. Reluctantly, I had the cortisone shot. I’ve had more than my share and didn’t want another one. But, I wanted to move on. Within a few weeks, I was back on track.
I persevered through 2 setbacks. I completed my rehab about 6-7 months post op. 99% of the time my shoulder is okay. I rarely have an issue and hope that nothing will make it flare in the future.
From this experience, I’ve learned to be extremely cautious while I’m recovering from surgery.
I wish you the best of luck in your rehab. I’m sure your firefighting community is looking forward to your return.
Feel free to share a future comment so others will see how long it took for you to recover.
The post is very useful, I will follow the advices. Thanks so much!
Vivian, Good Luck with your rehab.
I’m having decompression surgery on my left shoulder on Nov.1. I work for a garbage company, and have a cardboard route. My job requires pushing and pulling dumpsters around through snow, ice and everything else that lays on the ground. My work will only give me three months off. Am I going to be able to return to this kind of work after three months. Please help me.
Hi Rick, Your doctor is the best person to answer that question. He or she should be able to provide an estimated recovery time based on the pre and post surgery evaluations. Sometimes the surgeon will adjust the time table if the surgery ends up being different than anticipated or the rehabbing doesn’t follow the norm.
Keep in mind, that there are average healing times, but some people may recover/rehab quicker or slower based on different factors. If possible, try to avoid comparing yourself to others.
It’s crucial that you keep a positive attitude, ask questions whenever necessary, and follow the post rehab instructions. Hopefully, your recovery will go smoothly. Feel free to share your progress so others can benefit from your experience. Good Luck!
Hi i had a decompression surgery 6 years back and now i find that any exercise i do my shoulder starts to ach right up my neck.My arm is also shaking up to my hand,it also happens when i carry a bag or drive to long.Doctor is just referring me back to physiotherapy and this is happening more often now.
Sarah, I know how it feels to have pain years after a surgery. If you have a good relationship with your therapist, I would follow your doctor’s advice and have the therapist evaluate and treat the situation. If not, I’d consider either finding a new therapist or seeking a second opinion from another doctor. Since you’re experiencing significant discomfort that is affecting your quality of life, it’s essential that you find someone who can help. Good luck!
Sandra – so glad ? to have found your blog! I just scheduled my surgery to be done in four months (mid summer) and I’m scared out of my wits. You offered good advice which I appreciate. I’ve got a great PT gal and I trust my doctor – but I’ve never had major surgery so it’s daunting to think about what I’m putting myself into. But I’m tired of being in pain from this impingement so I guess it’s time to move forward!
Gail, Surgery should always be the last option. If nothing has worked to relieve your discomfort and pain, you have two options—live with the situation or try to rectify it. Yes, surgery can be scary and you’ll need to endure more pain before you see the light at the end of the tunnel. A positive attitude along with a competent surgeon and an effective physical therapist will help you through the process. Good Luck and keep me posted on your progress.
After 8 months of being in pain, trying a month of PT, a cortisone shot and having a very small ROM that whole time. I am now 9 days post op from a arthroscopic decompression surgery. Honestly the pain has not been as bad as I was expecting. I sat with the ice machine on 24/7 for the first 4 days and took pain meds on an every 6 hour schedule whether there was significant pain or not. My doctor and the recovery nurses stressed keeping above the pain with scheduled pain meds instead of catching up on the pain if not taking them. I did end up stopping the pain meds completely on day 6 post op due to horrible constipation. Now I’m taking Aleve when needed. I continue to use my ice machine all night and sleep in a recliner, I also ice it during the day if things feel achy in there. My post op appointment is 14 days post op. I’m assuming he’ll take out the staples. I’m curious if he will keep me in a sling or not. It’s my prominent arm/hand that is in a sling so it’s very hard to do some tasks. Sometimes I do end up moving that shoulder while doing something due to it being my prominent hand, I believe, but then I catch myself and tuck it back in the sling. It will be nice to have use of that hand again to eat, write, shower, dress, etc.
So far post op hasn’t been as bad as I was expecting. So hopefully it will continue. I can’t wait to get this sling off and into PT and get my arm back!
Janet, I’m glad to hear that your post op rehabbing is going well and that things are better than anticipated. I’m confident that as each week goes by you’ll continue to feel better. Don’t get discouraged if you hit a small bump along the road. Recovery is a process that unique to every individual. Good Luck!
Sandra – god bless you! I’m having surgery in about 5 weeks and I am concerned because I have to go back to work after two weeks. I was worried about pain since my surgery is on my dominant hand and I write and type all day. Where does one get an ice machine. What is it?
Sara,
If your doctor doesn’t provide the machine, you can do a online search for “ice machine for orthopedic surgery recovery.” The search will show multiple options.
Since everyone recovers at their own rate, it’s hard to predict how much pain you will experience when you need to return to work. I limited the amount of typing that I did post op. You may need to adjust your work load if typing makes your situation worse.
Good luck with your upcoming surgery.
I am 24 hours post-op. Not sure how to have to arm and shoulder. This shoulder splint has a loop for my thumb to sit in. I guess to take the weight off???? Not sure how to rest my arm with the loop.
Jodi,
If you’re not sure how to position your arm, I recommend calling the doctor’s office. I’m sure that they can guide you through the correct positioning. Good luck on your rehab. Best wishes for a speedy recovery.
Hi, thanks for taking the time to write this down! I am exactly one week post-op for subacromial decompression and distal clavical resection. My doctor gave me very little post-op instruction and I find that I am frustrated not knowing whether I am pushing it or babying it. How long should I expect to be in a sling? Refrain from driving? My ROM is basically two inches haha! Any movement to that point is fairly painful. My doctor’s initial discussion of the procedure said that people can be back in the gym within a week – I don’t feel that’s possible at all, but wonder then why I am still in pain. I don’t see the doctor for a post op appointment for another week and a half (2.5 weeks after procedure). I’m struggling to know what to do, what not to do, in the meantime in order to have the best outcome.
Bekka,
Rehab procedures vary from person to person and from doctor to doctor. Recovery time lines also have a range. There are many variables that are best addressed with medical team. If you have questions or concerns, I recommend that you contact your doctor’s office before your next appointment. Good luck in your recovery.
Hi, Sandra!! I’m beyond grateful for your blog. Thank you for taking the time to do this. I have subacromial decompression with bicep release surgery in a week. I’m seeking advice regarding the nitty-gritty after surgery. Unfortunately, I am no stranger to major surgeries. However, this will be my first that will limit my use of my dominant arm.
My issue is, I’m single and have two large dogs. While I do have offers of places to stay/go, I don’t want to burden anyone and it just seems like it will be easier for me to sleep in my own bed and have access to my own stuff. I plan on taking the dogs to a friend’s house for a few days post-surgery but thought I could manage dealing with ‘living’ on my own. I do have rides back and forth to the surgery and the post-op the day after. Do you think it’s manageable to recover solo or not so much??
Thank you SO much for your thoughts.
Hi Mari,
Thanks for your patience. I was out of the country with limited internet when you posted your comment. I hope that your procedure went well and the you are on the road to a full recovery. You are lucky to have friends who can provide assistance. Keep in mind that no two recoveries are ever the same. Post op usually has good and bad days. When in doubt, it’s always wise to contact your medical provider. Take care!
Hi I had shbracomoial.decompression 3 weeks ago and I am still in a lot of pain but it radiates down arm to fingers and also getting pain in collar bone and is slightly swelled ( I used to get this when driving for my job alot) Honestly say pain overall is worse than pain before op! Sleeping is the wors t. Spoke to physio just told me to take a nerve medication but no difference. Also when bend the arm and then straighten it it is so painful and stiff. Help any advice?
Janet, Thanks for your patience. I sincerely hope that over the last few weeks your pain has diminished and you are on the road to recovery. While everyone heals differently, it is always important to keep in contact with your doctor and physical therapist if something doesn’t seem quite right. Good luck with your recovery process.
Hi Sandra! I’m really grateful for your blog and article which is very detailed! I am scheduled for Subacramial Decompression arthroscopic surgery in 4 weeks and I’m very concerned about the post op pain/discomfort or possible set backs. I’m looking into buying an ice machine as well! Wish me luck. I’ll keep you posted on my progress. Thanks for the suggestions and sharing
Zorita,
Thanks for reaching out. I know that it is hard not to stress out before an upcoming surgery. Truthfully, there’s nothing you can do before the surgery other than purchase things like an ice machine, rearrange your schedule, make sure you have ample food and assistance, and that you have someone to drive you home from the procedure. Keep in mind that most people do not have setbacks. But like with any other surgical procedure it is important to have a positive attitude and to use common sense. Don’t do more than you are supposed to do and if something doesn’t seem right, contact your medical team asap. Good luck.